Shoulder pain can significantly impact your daily life. When this pain stems from arthritis, it can feel like a persistent, frustrating challenge. Many patients ask, “What can be done for arthritis in the shoulder?” The good news is that a wide spectrum of effective treatment options exists. These options range from simple lifestyle adjustments and physical therapy to surgical procedures. Understanding the possible treatment options can empower you to make informed decisions about your care.
Key Takeaways
- Non-surgical treatments like physical therapy and anti-inflammatory medications may provide relief for many patients.
- Surgery may be an option for advanced cases. When conservative treatments fail, procedures like total shoulder replacement or reverse total shoulder replacement aim to reduce pain and restore function.
- Many patients achieve meaningful pain relief and improved function by working with an experienced orthopedic specialist to create a personalized treatment plan that may evolve over time.
Understanding Shoulder Arthritis
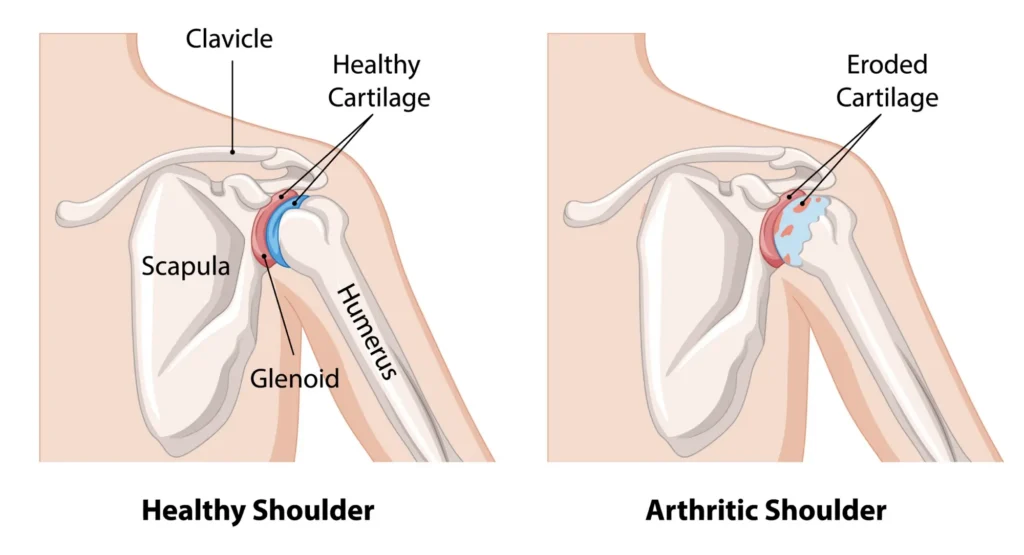
The shoulder is a complex ball-and-socket joint. It involves three bones: the humerus (upper arm bone), the scapula (shoulder blade), and the clavicle (collarbone). Arthritis can affect two main joints in the shoulder. The glenohumeral joint is the main ball-and-socket joint. The acromioclavicular (AC) joint is where the collarbone meets the shoulder blade.
In the shoulder, arthritis affects the smooth cartilage that covers the ends of the bones. This cartilage allows the bones to glide easily against each other. When arthritis develops, this protective layer begins to wear away. The result may be painful, bone-on-bone friction.
Types of Shoulder Arthritis
Several types of arthritis can affect the shoulder. Each type has a different cause and can respond differently to treatment.
1. Osteoarthritis (OA)
Osteoarthritis is the most common form of shoulder arthritis. It is often called “wear-and-tear” arthritis. OA typically develops slowly over time. It results from the gradual breakdown of joint cartilage and most often affects people over the age of 50. OA can affect both the glenohumeral and the AC joints.
2. Rheumatoid Arthritis (RA)
Rheumatoid arthritis is a systemic inflammatory disease. It affects the lining of the joints. It is an autoimmune disease, which means the body’s immune system mistakenly attacks its own healthy tissues. RA usually affects multiple joints throughout the body and often causes pain and stiffness that is worse after rest.
3. Post-Traumatic Arthritis
This type of arthritis develops after a shoulder injury. A fracture or dislocation can damage the joint surface. This damage can lead to cartilage breakdown years later. The initial injury sets the stage for future arthritic changes.
4. Rotator Cuff Tear Arthropathy
A massive, long-standing rotator cuff tear can lead to this form of arthritis. The torn tendons can no longer hold the head of the humerus in the socket. This causes the ball to move upward and rub against the acromion, and this abnormal joint contact destroys the cartilage.
Symptoms and Diagnosis
Recognizing the symptoms of shoulder arthritis supports early diagnosis, which allows for earlier intervention. Common symptoms include:
- Pain: The pain is usually described as dull and aching. It may become sharp with certain movements.
- Stiffness: The shoulder loses its range of motion, which makes it difficult to lift the arm or reach behind the back.
- Grinding or Catching: You may hear or feel a clicking, grinding, or snapping sensation, called crepitus. It can happen when rough cartilage surfaces rub together.
- Night Pain: Pain often interferes with sleep, and finding a comfortable sleeping position can become very challenging.
- Loss of Function: The ability to perform daily tasks decreases, as simple actions may become painful and difficult.
Making the Diagnosis
A thorough physical examination is the first step. Your doctor will typically assess your range of motion and strength, along with testing for tenderness.
Imaging tests may be used to support the diagnosis. X-rays are a common diagnostic tool. They show the amount of space between the bones and can also reveal bone spurs (bony growths that form around the joint).
Sometimes, your doctor may order an MRI or a CT scan. These advanced imaging tests provide more detail. They help evaluate the condition of the rotator cuff tendons and also show the amount of bone loss. This information can be especially important for surgical planning.
What Can Be Done for Arthritis in the Shoulder? Non-Surgical Treatments
For most patients, treatment begins with conservative, non-surgical methods. These approaches aim to manage pain and maintain function. They can be effective, especially in the early stages of arthritis.
1. Activity Modification and Lifestyle Changes
In this case, activity modification generally means avoiding activities that aggravate your shoulder pain. This often means limiting heavy lifting or repetitive overhead movements.
- Rest: Giving the joint a break during flare-ups can help reduce inflammation.
- Ice and Heat: Applying ice packs for 15 to 20 minutes may help reduce swelling and pain. Heat, such as a warm shower or heating pad, may relax stiff muscles.
- Assistive Devices: Using tools to help with reaching or gripping can lessen the strain on your shoulder.
2. Physical Therapy and Exercise
Physical therapy is frequently a cornerstone of non-surgical treatment. A physical therapist can design a specific exercise program for you that focuses on two main goals: maintaining range of motion and strengthening the surrounding muscles. Consistency is key to the success of physical therapy. In cases of severe arthritis, physical therapy may not be recommended.
3. Medications
Medications may be recommended to help control pain and inflammation. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) reduce both pain and swelling. Acetaminophen primarily targets pain. Always discuss medication use with your doctor.
4. Injections
When oral medications are not enough, in some cases, injections may be recommended:
- Corticosteroid Injections: These injections contain a strong anti-inflammatory medicine. They may provide months of relief.
- Emerging Biologic Treatments: Platelet-rich plasma (PRP) therapy is a newer option. It is a regenerative treatment that aims to harness the body’s natural healing abilities.
Surgical Solutions: When Conservative Care is Not Enough
When conservative treatments no longer provide adequate relief, surgery may become the next step. An experienced orthopedic surgeon can recommend a procedure based on the type of arthritis, the condition of your rotator cuff, and your activity goals.
1. Arthroscopy and Debridement
Arthroscopy is a minimally invasive surgical technique. The surgeon uses a small camera and instruments inserted through tiny incisions. This procedure is generally reserved for early-stage arthritis. It may also be used to cure AC joint arthritis.
During the procedure, the surgeon can:
- Remove Loose Bodies: Small fragments of cartilage or bone can cause catching and pain. The surgeon removes these fragments.
- Debride the Joint: They smooth rough cartilage surfaces and remove inflamed tissue.
- Treat Bone Spurs: They can remove bone spurs (osteophytes) that limit motion.
Arthroscopy can relieve pain and improve motion temporarily. It does not replace the damaged cartilage.
2. Total Shoulder Arthroplasty
Total shoulder replacement replaces both the ball and the socket, aiming to replicate the natural anatomy of the shoulder. The surgeon replaces the head of the humerus with a metal ball and covers the socket with a smooth plastic component. Total shoulder replacement generally works best when the patient has an intact, healthy rotator cuff, which powers and controls the new joint.

3. Reverse Total Shoulder Arthroplasty
The reverse total shoulder replacement is a specialized type of shoulder replacement. In this procedure, the anatomy of the joint is reversed. The metal ball is placed on the shoulder blade (glenoid). The plastic socket is placed on the upper arm bone (humerus). By changing the anatomy, this design enables the deltoid muscle to compensate for the rotator cuff. This procedure can be especially beneficial for patients with rotator cuff tear arthropathy, irreparable rotator cuff tears, and complex fractures.

Recovery and Rehabilitation
Regardless of the treatment path, recovery is a process that requires commitment and patience. Surgical recovery tends to be more structured. It typically involves a brief period of immobilization in a sling to protect the healing tissues. Physical therapy often begins soon after surgery.
The rehabilitation program generally progresses in phases:
- Passive Range of Motion: The therapist or your other arm moves the post-operative arm for you. The goal is to protect the surgical repair while preventing stiffness.
- Active Range of Motion: In this phase, you begin to move the operated arm on your own.
- Strengthening: You start exercises to rebuild muscle strength. Strengthening exercises may progress in intensity over time.
Full recovery after a shoulder replacement can take six months to a year or longer although many patients experience significant improvement within a few months.
Summary
Shoulder arthritis is a common condition that causes pain and loss of motion. Modern orthopedic medicine offers a wide range of solutions. Conservative, or non-surgical, treatment options may include physical therapy, medication, and injections. When these methods are no longer effective, surgical options may be recommended. These surgeries include total shoulder replacement and reverse total shoulder replacement. The ultimate goal is to reduce pain and restore function, helping you to return to the activities you enjoy.
Frequently Asked Questions
Can I still play sports after a total shoulder replacement?
Many patients return to low-impact sports after a total shoulder replacement. These activities may include golf, swimming, and tennis. High-impact sports or activities involving heavy (>50 pounds) overhead lifting or throwing are generally discouraged. Weight training is permitted and encouraged after surgery. Your surgeon will provide specific recommendations based on your recovery and the type of implant used.
What is the difference between a total and reverse shoulder replacement?
The difference lies in the joint’s anatomy. A total shoulder arthroplasty mimics the natural shoulder. It places the ball on the arm bone and the socket on the shoulder blade. A reverse shoulder arthroplasty flips this arrangement. It places the ball on the shoulder blade and the socket on the arm bone. Surgeons often use the reverse option when the rotator cuff is severely damaged or the shoulder is severely worn out.
What is the first sign of shoulder arthritis?
An early sign is often a deep, aching pain in the shoulder. This pain may be mild at first. It usually worsens with activity. Stiffness and a reduced ability to move the arm are also early indicators.


