Shoulder pain has a way of infiltrating every corner of your day. Whether reaching into a cabinet, buckling a seatbelt, or just sleeping through the night, tasks that used to be effortless can start to feel like challenges. When physical therapy, medications, and injections have run their course, and the relief just isn’t sticking, shoulder replacement surgery may enter the conversation. And with that comes a very honest, very understandable question: Is shoulder replacement worth it?
It’s not a decision to take lightly, and it’s not right for everyone. Whether it makes sense for you depends on your specific diagnosis, the severity of your symptoms, your overall health, and your goals for recovery. In this post, we’ll review the full picture, including the potential benefits, the process, and what recovery actually looks like, so that you can make an informed choice.
Key Takeaways
- Shoulder replacement surgery may offer significant pain relief and improved function for patients with severe shoulder joint damage.
- Two main types exist, total shoulder replacement and reverse shoulder replacement, and the right choice depends on your diagnosis and anatomy.
- Whether shoulder replacement is the right step for you requires a thorough evaluation and honest conversations with your shoulder surgeon.
Understanding the Shoulder Joint
The shoulder is the most mobile joint in the human body. It’s a ball-and-socket joint, where the rounded top of your upper arm bone (the humerus) fits into a shallow, cup-shaped socket in your shoulder blade called the glenoid. A smooth layer of cartilage cushions the surfaces where these bones meet, allowing fluid, nearly frictionless movement.
Over time, that cartilage can wear down. Osteoarthritis, inflammatory conditions like rheumatoid arthritis, previous fractures, and severe rotator cuff damage can all accelerate this process. When the cushioning is gone, bone may grind against bone. Pain sets in, often deep, persistent, and difficult to ignore. Range of motion and strength decline.
Shoulder replacement surgery removes the damaged joint surfaces and replaces them with carefully engineered artificial components. Think of it as replacing a severely worn hinge with a new, well-functioning one. The goal is to restore smooth, more pain-free movement and help you get back to the activities that matter most to you.
Who Might Be a Good Candidate?
Not every patient with shoulder pain needs surgery. Many cases can be meaningfully managed with conservative treatment, such as physical therapy, anti-inflammatory medications, activity modification, and targeted injections. Surgery may become a consideration when those approaches have been exhausted and quality of life remains significantly affected.
Patients who may be good candidates for shoulder replacement often share a few things in common:
- A confirmed diagnosis of shoulder arthritis, severe rotator cuff damage, or significant joint deterioration causing ongoing pain and disability
- Persistent symptoms that haven’t responded adequately to conservative care
- Pain that meaningfully disrupts daily activities, such as sleeping, dressing, working, or participating in recreational activities you value
- A genuine commitment to the recovery process, including physical therapy
Certain factors may make surgery less appropriate or require careful consideration, including poorly controlled medical conditions or insufficient bone quality. A thorough preoperative evaluation helps with identifying these factors early.
Two Types of Shoulder Replacement: What’s the Difference?
Shoulder replacement isn’t a single procedure. There are two main approaches, and selecting the right one depends heavily on the condition of your rotator cuff, the group of four muscles and tendons that stabilize and power your shoulder.
Total Shoulder Replacement
Total shoulder replacement, also called anatomic shoulder replacement, replaces both the ball and socket with components designed to replicate your natural joint anatomy. This approach typically works best when the rotator cuff is still intact and functional.
For total shoulder replacement, I use the Shoulder Innovations InSet® Total Shoulder System. What sets this system apart starts with the glenoid component, the socket side of the implant. Traditional glenoid implants sit on top of the bone surface, which can expose them to loosening forces over time. The InSet® glenoid component, by contrast, is placed within the bone rather than on top of it. This countersinking approach is designed to position the implant within the bone rather than on top of it, which may help optimize how forces are distributed across the joint. This distinction matters, as glenoid loosening is a known reason patients require revision shoulder surgery.

Both short-stem and stemless configurations are available, so I can select the option that best fits your specific anatomy.
Reverse Shoulder Replacement
Reverse shoulder replacement takes a fundamentally different structural approach. It literally flips the positions of the ball and socket components: the ball attaches to the shoulder blade side, and the cup attaches to the arm bone. It sounds counterintuitive, but the design can be highly effective for a specific group of patients.
Reverse replacement is generally recommended when the rotator cuff is severely damaged or entirely torn and can no longer adequately support anatomic joint function. By repositioning the center of the joint’s rotation, this design allows the deltoid muscle to compensate for the missing rotator cuff.

I perform reverse shoulder replacement using the InSet® Reverse Shoulder System. This design is intended to help manage stress at the bone-implant interface and support stable fixation over time.
Planning Your Surgery
One of the most meaningful advances in shoulder replacement over the past several years isn’t the implant itself; it’s our ability to plan the surgery with precision before the patient even enters the operating room.
Before your procedure, I use ProVoyance®, which takes CT scan data and converts it into a highly detailed, three-dimensional reconstruction of your specific shoulder anatomy. From there, I can assess your bone structure, evaluate any deformity or bone loss, and plan exactly how the implant components should be positioned, all tailored to your unique anatomy.
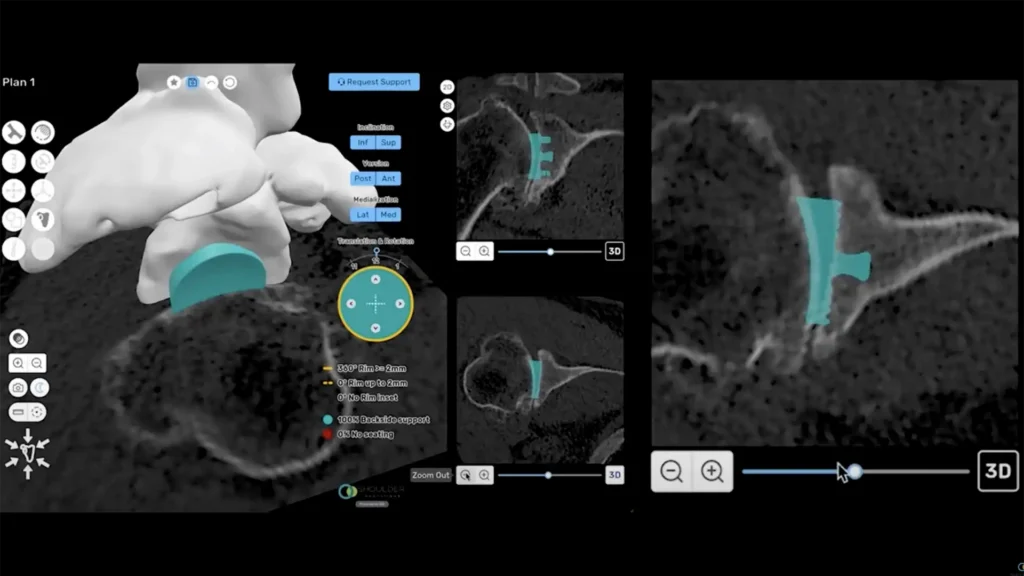
This kind of individualized preoperative planning helps guide implant selection, sizing, and placement decisions before we ever step into the operating room. This approach allows for highly detailed surgical planning tailored to your anatomy, which may help support accurate implant placement and alignment.
What Recovery Looks Like
Setting realistic expectations before surgery is one of the most important things we can do together. Recovery from shoulder replacement is a gradual process, not a quick turnaround. Understanding the timeline helps patients stay the course and ultimately get the most from the procedure.
In the weeks following surgery, most patients wear a sling to protect the healing joint. Physical therapy typically begins relatively soon after the procedure and continues for several months. The goal is to help restore range of motion, rebuild strength, and guide you back to the activities you’re aiming to return to.
Maximal recovery typically takes somewhere between six months to a year or longer, though individual timelines vary depending on age, health, and the complexity of the procedure. Many people return to light daily activities within a few weeks. More physically demanding activities follow at a pace that your recovery and your surgeon’s guidance will help determine.
Risks and Realistic Expectations
Like any surgical procedure, shoulder replacement carries risks worth understanding. These can include infection, blood clots, nerve injury, stiffness, and implant-related complications.
Results can also vary. Many patients who undergo shoulder replacement for appropriate reasons report significant, meaningful improvements in both pain and function. However, surgery doesn’t come with guarantees, and outcomes can be influenced by factors like overall health, bone quality, surgical complexity, and adherence to the rehabilitation program.
Before recommending surgery, an experienced shoulder surgeon should review your full medical history, imaging studies, and health status carefully. Identifying any factors that could affect your outcome allows for thoughtful planning and realistic goal-setting.
So, Is Shoulder Replacement Worth It?
For many patients, shoulder replacement has offered meaningful, lasting improvement. Pain relief can be substantial. Functional recovery may allow patients to return to activities they haven’t been able to enjoy for years.
Is shoulder replacement worth it for you specifically? That’s a question we need to answer together. It depends on your diagnosis, your goals, your health history, and an honest conversation about what the process involves and what outcomes are realistic for your situation. I don’t take a one-size-fits-all approach. Every patient I see gets a thorough evaluation, and we determine together whether surgery is the right path, and if so, which approach and technology offer you the best possible chance at a great outcome.
If shoulder pain has been limiting your life, it may be time to schedule a consultation. Understanding your options is always the right first step.
Summary
Shoulder replacement surgery has helped many patients reclaim their quality of life after years of chronic pain, stiffness, and functional decline. When the right patient is selected, the right procedure is chosen, and the surgery is planned and executed with precision, it can be a profoundly worthwhile intervention. Is shoulder replacement worth it? For many patients living with advanced shoulder joint damage, the answer may very well be yes.
Frequently Asked Questions
Can shoulder replacement be done as an outpatient procedure?
For appropriate candidates, outpatient shoulder replacement is increasingly common. Whether outpatient surgery is suitable for you depends on your overall health and other factors we’d evaluate together.
When can I return to sports or physical activity?
This varies by activity and by patient. Many people may return to low-impact activities like golf or swimming within several months. Higher-impact or contact activities may not be appropriate. We’ll discuss your specific activity goals as part of your recovery plan so expectations are clear from the start.
What’s the difference between total and reverse shoulder replacement?
Total (anatomic) shoulder replacement replicates your natural joint structure and works best when the rotator cuff remains intact and functional. Reverse shoulder replacement repositions the joint’s ball and socket to compensate for a severely damaged or absent rotator cuff, allowing the deltoid muscle to power shoulder movement. Your diagnosis and anatomy help determine which approach is appropriate for you.
What if conservative treatment hasn’t worked? Does that mean I definitely need surgery?
Not necessarily. Exhausting conservative treatment is generally a prerequisite for considering surgery, but it doesn’t automatically mean replacement is the next step. A thorough evaluation, including a review of your imaging, your symptoms, and your goals, helps us determine whether surgery makes sense and, if so, what type would serve you best.


