A broken shoulder, medically known as a shoulder fracture, is a common yet often debilitating injury. It can result from a variety of incidents, including falls, sports injuries, or high-impact trauma, and can significantly limit your ability to perform daily activities. In this post, we’ll take a closer look at causes, diagnosis, and how to treat a broken shoulder.
Key Takeaways
- A broken shoulder can involve the clavicle (collarbone), scapula (shoulder blade), or the proximal humerus (the top of the arm bone). The specific bone and fracture pattern heavily influence the treatment plan.
- Many shoulder fractures, particularly non-displaced or minimally displaced proximal humerus fractures, heal well with non-operative methods like immobilization and physical therapy.
- Surgical intervention is typically reserved for fractures that are significantly displaced, unstable, or involve the joint surface.
What Constitutes a Broken Shoulder?
The shoulder is a complex structure composed of three main bones that work together to provide an incredible range of motion. When people talk about a broken shoulder, they are usually referring to a fracture in one of these three bones:
The Scapula (Shoulder Blade): This is a large, flat, triangular bone located on the back of the rib cage. Scapular fractures are relatively rare and usually result from high-energy trauma, such as a motor vehicle accident.
The Clavicle (Collarbone): This long, slender bone connects the arm to the trunk of the body. Clavicle fractures commonly occur after a fall directly onto the shoulder or an outstretched arm.
The Proximal Humerus (Upper Arm Bone): This is the ball part of the ball-and-socket joint. Fractures here are most common in older adults, often due to osteoporosis and a fall from a standing height.
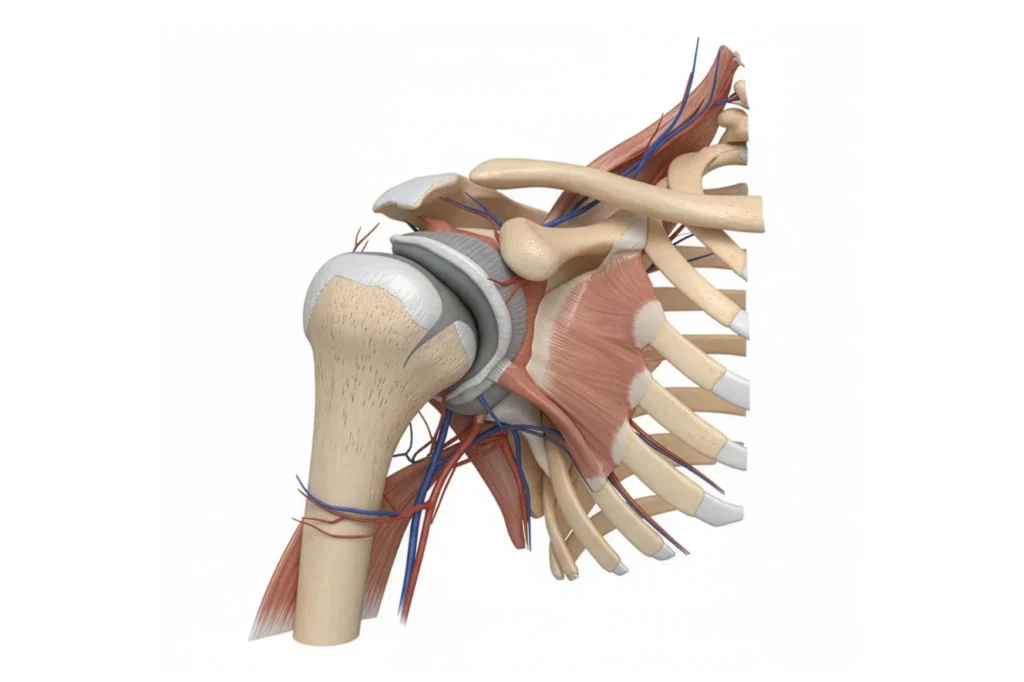
Each type of fracture presents unique challenges and requires a tailored approach.
Initial Steps: Diagnosis and Immediate Care
If you suspect you have a broken shoulder, seeking immediate medical attention is important. The initial evaluation will involve a physical examination and imaging studies. Your doctor will first assess your symptoms, which may include severe pain, swelling, bruising, and an inability to move the arm. They will also check for any signs of nerve or blood vessel injury.
Several imaging tests may be used to support or confirm the diagnosis:
- X-rays: Standard X-rays can provide clear images of the bone structure and help determine the location and severity of the break, including whether the fragments are displaced (moved out of alignment).
- CT Scans (Computed Tomography): For more complex fractures, especially those involving the joint surface (articular fractures) or the scapula, a CT scan may be necessary. This provides a detailed, three-dimensional view of the bone fragments.
- MRI (Magnetic Resonance Imaging): While not typically used for diagnosing the bone break itself, an MRI may be ordered to evaluate associated soft tissue injuries, such as rotator cuff tears or ligament damage.
Immediate Care
Before a definitive treatment plan is established, immediate care generally focuses on pain management and preventing further injury. This may involve:
- Immobilization: The arm is typically placed in a sling or a specialized shoulder immobilizer to keep the bone fragments stable and minimize movement.
- Pain Relief: Over-the-counter or prescription pain medications may be used to manage discomfort.
- Ice: Applying ice packs to the affected area may help reduce swelling and pain.
Non-Surgical Treatment: The First Line of Defense
For many patients, particularly those with non-displaced or minimally displaced fractures, the answer to how to treat a broken shoulder does not involve surgery. The goal of non-surgical treatment is to allow the bone to heal naturally while maintaining the best possible alignment and preventing stiffness.
1. Immobilization: The initial phase frequently involves wearing a sling or immobilizer for a period, with the timeline depending on the fracture type and individual health factors. The sling supports the arm and prevents movements that could disrupt the healing process.
2. Early Gentle Motion: While the fracture needs time to heal, prolonged immobilization can lead to shoulder stiffness. Your doctor or physical therapist will likely recommend starting very gentle, passive range-of-motion exercises for the elbow, wrist, and fingers to prevent stiffness in those joints.
3. Physical Therapy: This is typically a key component of non-surgical recovery. Once the orthopedic specialist confirms that the fracture has achieved sufficient stability, a formal physical therapy program may begin. It generally starts with passive range of motion, where the therapist moves your arm for you, and progresses in intensity over time.
Surgical Treatment: When is it Necessary?
Some fractures may require surgery to achieve a stable, functional outcome. The decision to operate is based on several factors, including the type of fracture, the degree of displacement, the patient’s age, and their functional demands.
Indications for Surgery
Surgery may be considered when the fracture is:
- Significantly Displaced: The bone fragments are far apart or severely misaligned, making it unlikely they will heal correctly on their own.
- Unstable: The fracture pattern is inherently unstable, meaning the fragments are likely to shift even with immobilization.
- Intra-Articular: The fracture extends into the joint surface, which can lead to arthritis if not perfectly realigned.
- Open (Compound): The bone has broken through the skin.
- Associated with Neurovascular Injury: Surgery may be needed to repair damaged nerves or blood vessels.
Common Surgical Procedures
The surgical approach varies depending on the specific bone and fracture pattern.
1. Open Reduction and Internal Fixation (ORIF): This is a common procedure for many displaced fractures of the clavicle and proximal humerus. The surgeon makes an incision to manually reposition (reduce) the bone fragments into their correct anatomical alignment. Once aligned, the fragments are held in place using specialized orthopedic hardware.
2. Intramedullary Nailing: This technique may be used for certain types of clavicle or humerus shaft fractures. A metal rod (nail) is inserted down the center (medullary canal) of the bone across the fracture site. This aims to provide strong internal support.
3. Arthroplasty (Joint Replacement): For complex proximal humerus fractures, especially in older patients with poor bone quality, the blood supply to the bone fragments may be compromised. In these cases, a reverse shoulder replacement may be the recommended option.
Summary
A broken shoulder is a serious injury, but with the right diagnosis and a committed approach to treatment, many patients can recover function. Whether your specialist recommends non-operative care with a focus on early motion and physical therapy, or a surgical procedure to restore alignment, your active participation is key.
Frequently Asked Questions
How long does it take for a broken shoulder to heal?
Timelines may vary between patients. The initial healing phase, where the bone fragments become stable enough to begin active motion, typically takes around 6 to 12 weeks. However, full recovery can take anywhere from four to nine months, and sometimes longer for complex injuries or surgical cases.
Will I need surgery for my broken shoulder?
Not necessarily. The majority of shoulder fractures are treated non-surgically, especially if the bone fragments are not displaced. Surgery is generally reserved for unstable, severely displaced, or open fractures. An experienced orthopedic surgeon can determine the best course of action based on your specific fracture pattern.
What is the difference between a broken shoulder and a dislocated shoulder?
A broken shoulder (fracture) involves a break in one of the bones (clavicle, humerus, or scapula). A dislocated shoulder occurs when the ball of the humerus pops out of the socket (glenoid). While they are distinct injuries, they can sometimes occur together.


